Varicocele, a common condition characterized by the enlargement of veins within the scrotum, can negatively affect testicular function and size, often leading to testicular atrophy.
This atrophy, or shrinkage of the testicle, raises concerns regarding fertility and hormonal health in affected individuals. A critical question in both clinical practice and patient care is whether testicular atrophy resulting from a varicocele is reversible, particularly following surgical or non-surgical intervention. This topic explores the potential for recovery of testicular size and function, reviewing current evidence and clinical outcomes.
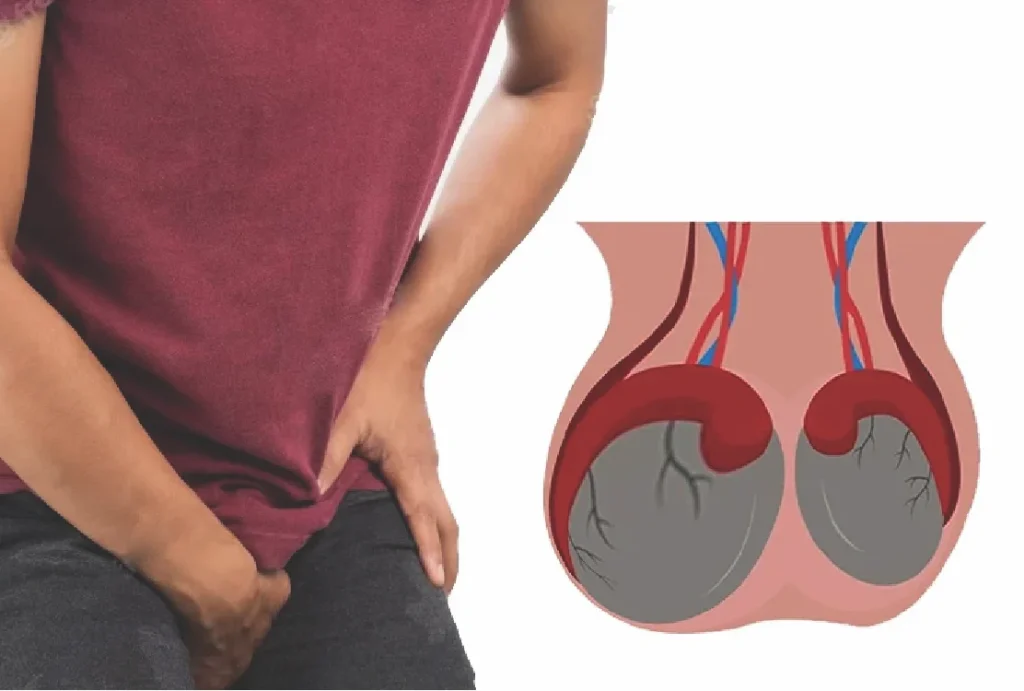
What is varicocele induced testicular atrophy?
Varicocele-induced testicular atrophy refers to the shrinkage or reduction in size of the testicle that occurs as a result of a varicocele — an abnormal enlargement of the veins within the pampiniform plexus in the scrotum.
This form of atrophy is most commonly seen in adolescents and young adult males, and its reversibility depends on several factors, including duration, severity of the varicocele, and whether treatment is initiated.
Causes
Varicocele-induced testicular atrophy is primarily caused by the physiological and biochemical changes that occur due to impaired venous drainage in the testicular veins. Below are the main mechanisms:
1. Increased Scrotal Temperature
- The pooling of blood in dilated veins raises the local temperature around the testicle.
- Testicular function, especially sperm production, is highly temperature-sensitive.
- Chronic elevation in temperature damages Sertoli cells, which support sperm development, leading to atrophy.
2. Hypoxia (Reduced Oxygen Supply)
- Poor circulation due to venous congestion limits oxygen delivery to testicular tissue.
- This oxygen deprivation harms germ cells and Leydig cells, impairing both sperm production and testosterone synthesis.
3. Oxidative Stress
- Varicocele increases the production of reactive oxygen species (ROS).
- These ROS damage cell membranes, DNA, and proteins in testicular tissue.
- Oxidative damage is a major factor in cell death and testicular shrinkage.
4. Hormonal Disruption
- Varicoceles can affect the local hormonal environment of the testis.
- Disrupted testosterone production or impaired responsiveness to gonadotropins can contribute to testicular dysfunction and volume loss.
5. Backflow of Toxic Substances
- Retrograde blood flow can carry renal or adrenal metabolites back into the testicular vein.
- These substances may be toxic to testicular tissue and contribute to cellular damage and atrophy.
6. Mechanical Pressure
- Dilated veins can exert pressure on the testicular parenchyma, compressing tissue and interfering with blood flow, leading to long-term structural damage.
Is varicocele-induced testicular atrophy reversible?
Yes, varicocele-induced testicular atrophy can be reversible in some cases, especially when detected early and appropriately treated, but the outcome depends on several factors.
Factors Favoring Reversibility:
- Early Diagnosis and Treatment
- Atrophy that is recent or mild responds better to treatment.
- Delayed treatment may result in irreversible damage to testicular tissue.
- Effective Surgical Correction (Varicocelectomy)
- Surgery to repair the varicocele (usually via microsurgical varicocelectomy) often leads to:
- Improved blood flow
- Lower scrotal temperature
- Reduction in oxidative stress
- Studies show partial or full recovery of testicular volume in many patients post-surgery, especially adolescents and young men.
- Surgery to repair the varicocele (usually via microsurgical varicocelectomy) often leads to:
- Younger Age
- Younger patients, particularly adolescents, tend to have a better regenerative capacity in testicular tissue.
- Absence of Severe Underlying Conditions
- If no other fertility or hormonal disorders are present, chances of recovery improve.
When Reversibility Is Less Likely:
- Long-standing varicoceles with prolonged atrophy
- Severe loss of testicular tissue
- Delayed intervention, particularly after years of damage
- Coexisting fertility issues or non-varicocele causes of atrophy
Clinical Evidence:
- Several studies report that testicular volume increases by 10–30% after varicocelectomy in men with atrophy.
- Improvement in sperm quality and hormonal levels is also documented in many cases.
Summary:
If varicocele is detected during adolescence (before the age of 17–18) and treated appropriately, the atrophy can regress. In surgeries performed later in adulthood, testicular atrophy does not reverse. Therefore, varicocele detected during childhood must be surgically treated.
Complications
Varicocele-induced testicular atrophy can lead to several short- and long-term complications, primarily related to fertility, hormonal balance, and testicular function. Below are the key complications:
1. Male Infertility
- One of the most significant complications.
- Atrophy impairs spermatogenesis (sperm production), leading to:
- Low sperm count (oligospermia)
- Poor sperm motility (asthenospermia)
- Abnormal sperm morphology
- Many men with unexplained infertility are later found to have a varicocele-related testicular issue.
2. Hormonal Imbalance
- The testicle plays a major role in testosterone production.
- Atrophied testes may produce less testosterone, leading to:
- Low libido
- Erectile dysfunction
- Fatigue
- Mood disturbances
- Reduced muscle mass and bone density (in long-term cases)
3. Persistent or Worsening Atrophy
- If left untreated, varicocele can cause progressive shrinking of the affected testicle.
- This may lead to permanent loss of function.
4. Scrotal Pain or Discomfort
- Some individuals experience chronic dull or aching pain due to the dilated veins and pressure buildup.
- Pain may worsen with physical activity or standing for long periods.
5. Testicular Asymmetry and Psychological Impact
- Visible difference in testicle size can cause:
- Body image concerns
- Embarrassment or anxiety, especially in adolescents and young adults
- Low self-esteem or sexual confidence
6. Suboptimal Response to Fertility Treatments
- In cases where the testicle is severely atrophied, even assisted reproductive techniques (like IVF or ICSI) may be less effective if sperm quality is poor.
Treatment
The primary goal in treating varicocele-induced testicular atrophy is to correct the underlying varicocele, restore normal testicular function, and prevent further damage. Treatment options vary depending on the severity of atrophy, age of the patient, symptoms, and fertility goals.
🩺 1. Conservative Management (Observation)
When used:
- Mild varicocele with no significant symptoms
- No evidence of testicular atrophy progression
- Normal semen parameters and hormone levels
Includes:
- Regular follow-up with scrotal ultrasound
- Semen analysis and hormonal testing
- Lifestyle changes (avoiding heat exposure, tight underwear)
⚠️ Observation is not recommended if testicular atrophy is already present or progressing.
🏥 2. Surgical Treatment (Varicocelectomy)
Most effective treatment for reversing or halting atrophy, especially in adolescents or young adults.
Types of Surgery:
- Microsurgical subinguinal varicocelectomy (most effective, lowest recurrence)
- Laparoscopic varicocelectomy
- Open inguinal or retroperitoneal approaches
Benefits:
- Improved testicular volume (especially in adolescents)
- Better sperm parameters
- Increased testosterone levels in some men
- May halt or reverse testicular shrinkage
Risks:
- Recurrence
- Hydrocele formation
- Rarely, injury to testicular artery
💉 3. Percutaneous Embolization
A minimally invasive, non-surgical option done via a catheter to block abnormal veins.
Benefits:
- Shorter recovery
- No incision
- Useful for patients unfit for surgery
Limitations:
- Requires experienced interventional radiologist
- Slightly higher recurrence rate compared to surgery
🧬 4. Hormonal or Fertility Support (Adjunctive)
May be considered after varicocele repair in men with persistent issues:
- Clomiphene citrate or aromatase inhibitors (to boost testosterone)
- Antioxidants (e.g., CoQ10, vitamin C, E) to reduce oxidative stress
- Assisted reproductive techniques (ART) in severe fertility cases
🔄 Can Atrophy Be Reversed?
- Yes, especially in adolescents and early-stage cases.
- Studies show testicular volume recovery in 60–80% of young patients after varicocelectomy.
- In adults, improvement is possible, though less predictable.
Prognosis
The prognosis of varicocele-induced testicular atrophy depends on several factors, including patient age, severity and duration of the varicocele, and timing of intervention. While testicular atrophy may be partially or fully reversible in some cases, in others, the damage may be permanent.
Key Prognostic Factors
| Factor | Effect on Prognosis |
| Age at diagnosis | Better outcomes in adolescents and young adults due to greater tissue recovery |
| Severity and duration | Long-standing, high-grade varicoceles have poorer recovery potential |
| Timeliness of treatment | Early surgical correction offers the best chance of reversing atrophy |
| Baseline testicular function | More favorable if hormone levels and sperm parameters are still within normal limits |
| Type of treatment used | Microsurgical varicocelectomy offers the highest success and lowest recurrence rate |
Favorable Prognosis:
- Early intervention, especially in adolescents
- Mild to moderate atrophy
- Improvement in testicular volume, sperm quality, and testosterone levels post-surgery
- Studies show 60–80% of adolescents experience partial or full recovery in testicular size after varicocelectomy
Poor Prognosis:
- Delayed treatment (after years of atrophy)
- Severe or complete testicular shrinkage
- Coexisting causes of infertility or hormonal disorders
- Lack of improvement in semen parameters post-surgery
Outcomes After Treatment:
| Parameter | Expected Outcome After Surgery |
| Testicular volume | May increase in 60–80% of young patients |
| Sperm count/motility | Improvement in 50–70% of cases |
| Testosterone levels | Mild to moderate improvement in many adults |
| Fertility (natural conception) | Higher success rates in couples with no other issues |
| Risk of recurrence | Low with microsurgical repair (<5%) |
Overall Prognosis:
Varicocele-induced testicular atrophy has a good prognosis if treated early, particularly in younger patients. Once permanent damage has occurred, reversal is unlikely, but fertility can often still be supported with medical or assisted reproductive techniques.
Summary
Varicocele-induced testicular atrophy can be partially or fully reversible, especially when diagnosed and treated early. Microsurgical varicocelectomy is the most effective treatment, with studies showing improvement in testicular volume in many patients, particularly adolescents and young adults. However, long-standing or severe atrophy may cause irreversible damage, making timely intervention crucial for optimal outcomes.
Prof. Dr. Emin ÖZBEK
Urologist
Istanbul- TURKIYE



Leave a Reply